If you have any questions please call
(03) 9898 4216
New patients welcome.
Please bring a referral from – GP or Specialist.
What is knee replacement surgery?
Total knee replacement surgery involves replacing parts of the knee joint which are damaged, arthritic or diseased with artificial metal and plastic components (known as a prosthesis). The prothesis enables the knee joint to move naturally.
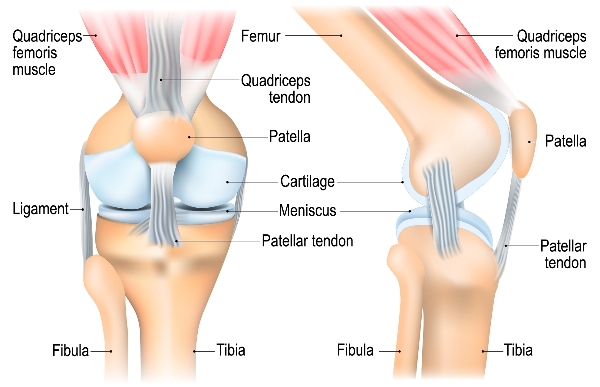
The knee is the largest joint in the body. It comprises of the lower part of the thighbone (femur) and upper part of the shinbone (tibia) as well as the kneecap (patella).
Covering all three bones is a smooth coating called cartilage which protects the bones and enables them to move easily.
Dr Riazi uses robot-assisted computer navigation, 3-D printed templates and the latest technology to prepare patient tailored and specific implants with high flexion or bendability.
Why consider knee replacement surgery?
Severe knee pain from arthritis or joint damage can make everyday tasks like walking, climbing stairs, or even resting difficult.
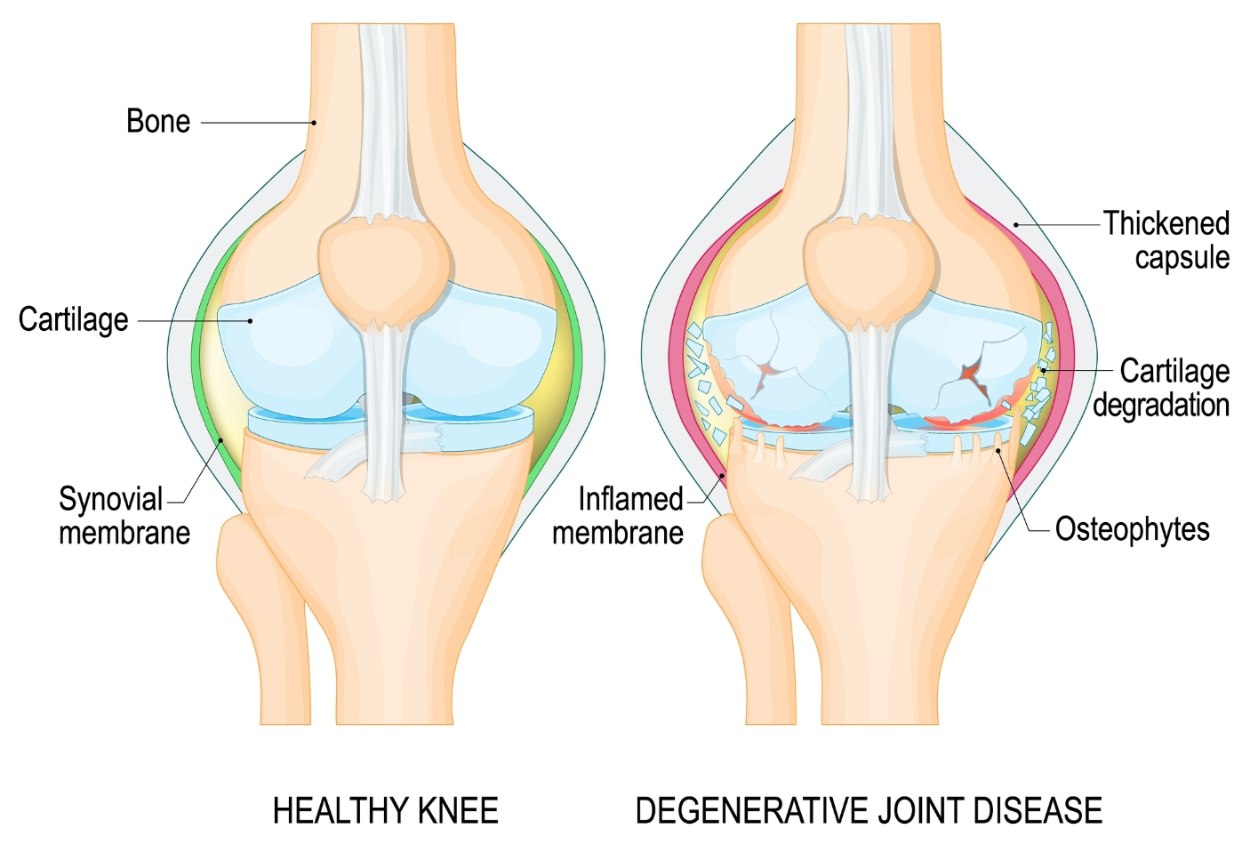
Arthritis is the most common cause — as the knee cartilage wears away, the joint becomes stiff, swollen, and painful, eventually limiting your ability to walk and stay active.
Dr Riazi will first explore non-surgical options with you, such as pain medication, walking aids, weight management, or temporary injections to ease pain and inflammation.
If these no longer provide relief, a total knee replacement may be recommended. The main benefit is long-term pain relief, along with better mobility and quality of life after surgery and rehabilitation.
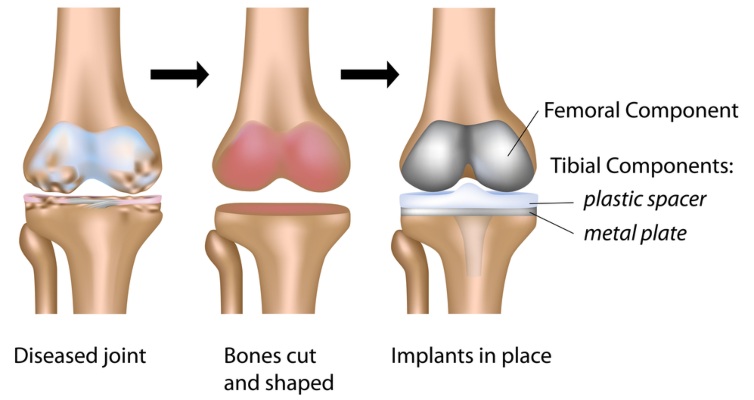
What happens during knee replacement surgery?
Before surgery – Your anaesthetist will assess you and recommend the most appropriate form of anaesthesia. In most cases, a general anaesthetic is used so you’re fully asleep, though a spinal anaesthetic with local anaesthetic and sedation is an equally safe alternative.
Before surgery, Dr Riazi will meet with you to answer any questions and mark the surgical site.
Every knee is unique, and Dr Riazi selects from a range of implant sizes to ensure the best fit. A tourniquet is placed around the upper thigh to reduce blood loss. Pre-operative planning includes advanced 3-D modelling or computer-assisted navigation, allowing precise alignment of the knee replacement for optimal function and long-term results.

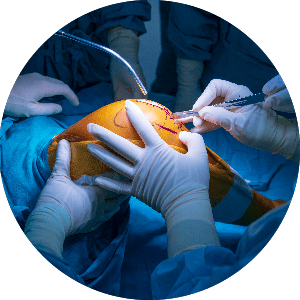
Once the optimal fit is confirmed, Dr Riazi implants the final prosthesis, with or without bone cement. He checks that the knee moves smoothly and is properly aligned before closing the incision with dissolvable sutures and applying a dressing.
The procedure takes around two hours. All patients receive intravenous antibiotics before and after surgery to reduce infection risk. You’ll wake in the recovery room and stay there briefly before being transferred to the ward.
Preparing for knee replacement surgery
Please ensure to let Dr Riazi know about any medical conditions you may have. You will be referred by Dr Riazi to a Perioperative Physician, who will assess your overall health and fitness to undertake surgery and anaesthesia. You may need to have some pre-operative tests such as blood tests, an echo-cardiogram and/or a chest x-ray.
1. Your Medications and Surgery – It is very important that Dr Riazi knows about all the medicines you are taking before your surgery. This includes:
All over the counter and prescription medicines
- Over-the-counter medicines (such as pain relief or cold tablets)
- Herbal or natural supplements
- Vitamins
- Weight loss medications (such as Ozempic®, Wegovy®, Saxenda®, Mounjaro® and others)
Please bring a written list of all your medications (or bring the boxes/bottles) to your consultation, and when you come into hospital for your surgery. This helps ensure your operation and treatment is safe and well-planned.
2. Smoking – Smoking increases your risk of complications during and after surgery, including infection. Quitting before your procedure and staying smoke-free aids healing and improves overall health. If you smoke, now is the perfect time to quit—speak to your GP for support.
3. Keeping fit – It is important to try and be as fit as possible before surgery to reduce the chance of complications and reduce the length of recovery. If it is difficult to move around then a gentle exercise such as swimming and hydrotherapy are good options.
4. Fasting – Dr Riazi’s team will guide you on fasting. Generally, fast from midnight for morning surgery, or from 6am for afternoon surgery. Clear fluids are allowed up to 4 hours before the procedure.
5. Home Preparation – There are a number of measures you can take to prepare for coming home after surgery.
- Furniture – Make sure you can easily move throughout your home
- Trip hazards – Remove any rugs or throws that may cause a fall
- Special equipment – Shower chair, handrails or raised toilet seat.
- Single floor living space – Walking up and down stairs may be difficult during early recovery
- Household chores assistance – Plan ahead for cooking and shopping
- Freeze some meals – Have food you can prepare quickly and easily or arrange for someone to bring you meals.
Knee replacement surgery – Potential complications
Bleeding – Some blood loss can occur during surgery, and a transfusion may occasionally be needed.
Venous Thromboembolism (VTE) – A blood clot may form in a vein (DVT) or travel to the lungs (PE). To reduce risk, you’ll receive blood-thinning medication, compression stockings, and early mobilisation support.
Infection – You’ll receive antibiotics during and after surgery to help prevent infection. If an infection develops, further treatment will be provided.
Pain – Some pain is expected. Dr Riazi’s team uses advanced pain management, combining medications safely, to ensure comfort, and support early movement.
Anaesthesia Risks – Your anaesthetist will discuss options and any associated risks before surgery.
Knee Stiffness – Temporary knee stiffness is common, and usually improves with exercise and reduced swelling.
Nerve, Ligament or Vessel Injury – Rarely, these may be damaged during surgery, causing bruising, weakness, or numbness, usually temporary but occasionally permanent.
Dislocation – Extremely rare, when the knee joint surfaces lose contact.
Leg Length Difference – The operated knee may appear slightly longer due to straightening, this is normal and unavoidable.
Post-Operative Recovery
After your operation
You’ll recover briefly before moving to the surgical ward, where nursing staff will care for you. Early movement is encouraged to speed recovery and reduce blood clot risk. A physiotherapist will assist you in getting out of bed and walking—often the same day or the day after surgery—and support you until you’re moving independently.
Active recovery participation
Your active participation is vital to a successful recovery. Follow the advice of Dr Riazi and his team both in hospital and at home. The physiotherapist will teach you strengthening exercises that may cause some discomfort or swelling—take your prescribed painkillers as directed to stay comfortable and mobile.
At home, expect some pain and swelling for a few weeks. Use ice packs and elevate your leg with a pillow under your heel (not your knee) to reduce swelling. Change your knee position every hour while awake to prevent stiffness and aid recovery.
Post operative wound care instructions
- Most wounds are closed with dissolving stitches, which do not need to be removed.
- The dressing applied in the operating room is the most sterile, so it is important to keep it on for 10–14 days. Please do not remove or change the dressing yourself.
- Some wounds are covered with surgical glue, which helps reduce wound ooze.
- Contact our rooms or the hospital ward if the dressing becomes soaked or if you notice any unusual bleeding or oozing.
Follow-up checks
Joint replacement (arthroplasty) patients – Routine wound checks are usually not required. You may remove your dressing at 2 weeks or book an appointment with your GP at that time for a wound check if preferred.
Exercises
You will be given a regimen of exercises to perform by your physiotherapist. You should aim to do 30 minutes of exercise two to three times a day. These are very important for your recovery.
Walking
By discharge, you’ll be walking short distances safely with a walker, crutches, or a stick. Gradually increase your movement and reduce reliance on aids—most patients progress from a walker to a stick within a few weeks. Walking is excellent exercise and will become easier as your new knee strengthens and settles.
Driving
You can normally start to drive around 6 weeks after surgery as this will be when most patients are comfortable walking.
KNEE REPLACEMENT SURGERY MELBOURNE
Dr Riazi consults with public and private orthopaedic patients from all over Melbourne. Public patients – Epworth Eastern Hospital – 12th Floor – Suite 12.4, 1 Arnold Street, Box Hill, VIC 3128. Public patients – Box Hill Hospital, 8 Arnold Street, Box Hill, VIC 3128. He also has a private consulting location at Adeney Private Hospital, 209 Cotham Road, Kew Vic 3101.